31 Provider Satisfaction Survey Questions
Explore 25 provider satisfaction survey questions with sample templates, best practices, and insights to improve care and patient feedback.
Provider satisfaction survey questions help you measure how supported, heard, and effective your clinical team feels. Depending on your organization, “provider” may mean physicians, APPs, nurse leaders, behavioral health providers, or other licensed clinicians.
Why provider satisfaction matters
Here’s the thing: when providers are satisfied, you’re more likely to improve retention, reduce burnout, strengthen patient experience, boost care quality, and run operations more smoothly, which can also help financial performance. Plus, this guide walks you through survey types, when to use each one, sample questions, and how to turn feedback into real improvements instead of letting it collect dust.
Overall Provider Satisfaction Survey Questions
Sample questions
How satisfied are you overall with your experience as a provider in this organization?
How likely are you to recommend this organization to other providers as a place to work?
To what extent do you feel supported in delivering high-quality patient care?
How satisfied are you with communication from organizational leadership?
How likely are you to remain with this organization over the next 12 months?
Big-picture pulse check
Why & When to Use
Use this survey type when you want a broad read on how providers feel across your organization, without diving into every issue all at once.
It works especially well for annual or biannual benchmarking, leadership reporting, and spotting high-level trouble areas before you send more targeted follow-up surveys.
Plus, it is especially helpful during growth periods, restructuring, leadership transitions, or after major policy updates, when provider sentiment can shift fast and quietly. Think of it as your organizational weather report, minus the dramatic storm music.
Keep the survey short enough that busy providers will actually finish it, but broad enough to reveal meaningful trends over time.
A simple setup often works best:
Use Likert scales for satisfaction.
Use agreement scales for support, communication, and trust.
Add one or two open-ended follow-ups to catch context numbers cannot explain.
On top of that, pair broad satisfaction questions with one or two diagnostic questions so you can tell what is driving the scores.
You will also get more useful insights if you segment results by:
Specialty
Tenure
Location
Employment model
Here's the thing: one overall score is helpful, but segmented data shows you where attention is actually needed.
Physician intent to leave is negatively associated with job satisfaction, supporting overall satisfaction and retention questions in provider surveys (source).
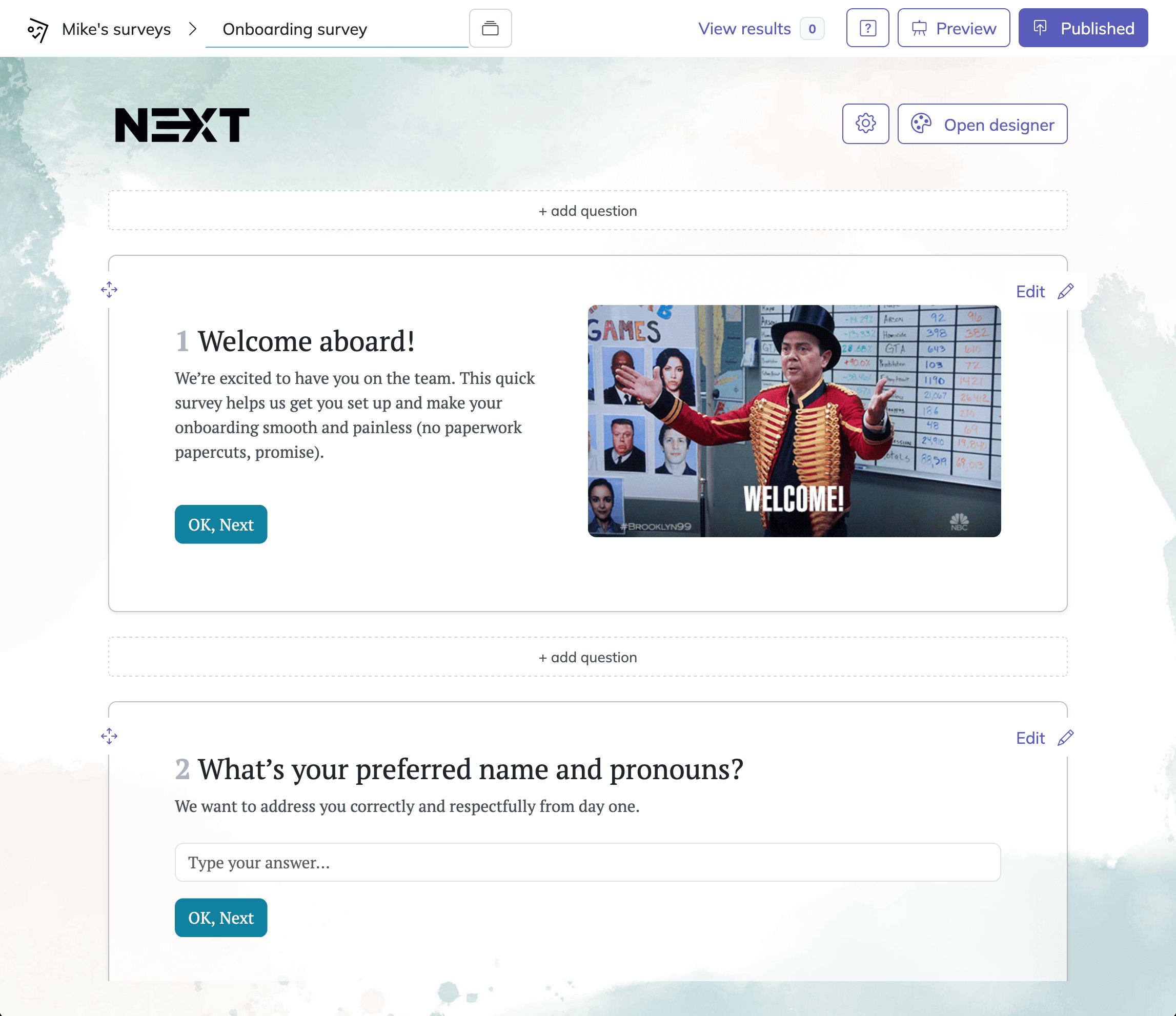
How to create a provider satisfaction survey in HeySurvey
1. Create a new survey
Start by opening a provider satisfaction survey template, or create a new survey from scratch if you want full control. HeySurvey lets you begin without an account, so you can explore the editor first. If you already have your own title, give the survey a clear internal name, such as “Provider Satisfaction Survey,” so it is easy to find later.
2. Add questions
Click Add Question to build your survey. For provider satisfaction surveys, use choice or scale questions for ratings, such as communication, wait time, professionalism, and overall experience. Add a few text questions for comments or suggestions. You can mark important questions as required and reorder them anytime. If needed, use one question per page for a cleaner experience.
3. Publish survey
Before sharing, click Preview to check how the survey looks on desktop and mobile. When everything is ready, click Publish to create a shareable link. You can then send it to patients or embed it on your website.
Provider Work Environment and Culture Survey Questions
Sample questions
Do you feel respected by colleagues, staff, and leadership in your day-to-day work?
How satisfied are you with the level of teamwork within your department or practice?
Do you feel psychologically safe speaking up about concerns or mistakes?
How well does the organization’s culture align with your professional values?
How satisfied are you with the organization’s recognition of provider contributions?
Culture shapes everything
Why & When to Use
Use this survey type when you want to understand whether your workplace culture truly supports provider well-being, collaboration, and trust.
It is especially useful when retention starts slipping, morale feels off, or teams mention communication, respect, or teamwork problems more often than you would like.
Here’s the thing: culture problems often push providers out the door even when pay and benefits look perfectly competitive on paper. A healthy culture keeps people engaged, while a messy one can make even a good job feel like a group project gone wrong.
This survey is also valuable after mergers, staffing shifts, leadership changes, or culture-improvement efforts, when day-to-day dynamics can change fast.
To get more honest and useful feedback, keep confidentiality front and center and say clearly how responses will be protected.
Plus, add optional comment fields so providers can share examples of positive and negative workplace behaviors in their own words.
A few practical ways to strengthen this survey:
Pair it with retention data to spot culture patterns behind turnover.
Review it alongside exit interview findings for added context.
Include questions about respect, recognition, safety, and teamwork, not just general satisfaction.
Leave space for comments, because culture issues usually live in the details.
In a national survey of English general practices, a more favorable team climate was associated with higher staff job satisfaction, better retention, and lower burnout (source).
Provider Workload, Staffing, and Burnout Survey Questions
Sample questions
How manageable is your current patient load and overall workload?
Do you have adequate staffing support to provide safe, effective care?
How often do you feel emotionally exhausted because of your work?
How satisfied are you with your schedule, call coverage, or shift distribution?
Do you have enough time to complete documentation and administrative tasks during normal working hours?
Burnout usually whispers before it shouts
Why & When to Use
Use this survey type when you need a clear read on workload pressure, staffing gaps, scheduling strain, and burnout risk before they turn into bigger problems.
It works especially well when you are seeing more absenteeism, lower engagement, slower productivity, or higher provider turnover.
Here’s the thing: a busy week is normal, but chronic overload is a different beast entirely, and it tends to leave clues long before people formally complain.
This survey is especially useful after patient census increases, scheduling changes, documentation demands, or service line growth, when work expands faster than support systems do.
On top of that, it helps to measure both operational strain and emotional exhaustion, because one tells you what is happening and the other tells you what it is costing your people.
A few practical ways to make this survey more useful:
Ask about patient load, staffing coverage, admin time, and scheduling fairness.
Include burnout indicators like emotional exhaustion, not just workload satisfaction.
Run it more often than a once-a-year survey if burnout risk is rising.
Use results to improve staffing models, scheduling policies, and workflow design.
Plus, if your providers are charting at dinner, that is not efficiency, that is a flashing dashboard light.
Provider Leadership and Communication Survey Questions
Sample questions
How effectively does leadership communicate decisions that affect your work?
Do you feel your feedback is heard and acted on by leaders?
How much trust do you have in organizational leadership?
How clear are leaders about priorities, expectations, and organizational goals?
How satisfied are you with the timeliness and transparency of internal communication?
Good communication does not erase hard decisions, but it does make them easier to trust
Why & When to Use
Use this survey type when you want to understand how providers view leadership trust, transparency, responsiveness, and communication around decisions that shape daily work.
It is especially useful when providers feel disconnected from leadership, unsure about priorities, or left guessing about why changes are happening.
Here’s the thing: people can live with an unpopular decision more easily than a confusing one.
This survey works well after policy changes, leadership transitions, mergers, restructuring, or any stretch of organizational uncertainty where rumors start doing cardio before facts arrive.
On top of that, it helps you separate communication issues by leadership level, because immediate supervisors, medical leadership, and executive leadership are not always experienced the same way.
A few practical ways to make this survey more useful:
Ask separately about frontline managers, physician or clinical leaders, and executive leadership.
Measure clarity, timeliness, transparency, and whether feedback leads to visible action.
Use the survey before and after change readiness survey questions efforts to spot trust shifts over time.
Share the results back with providers, along with next steps, so the survey itself builds credibility instead of eye-rolls.
Plus, when people never hear what happened after they gave feedback, trust tends to pack a suitcase.
In a 2015 Mayo Clinic survey, each 1-point increase in physician-supervisor leadership score was linked to 9.0% higher physician satisfaction and 3.3% lower burnout (source).
Provider Compensation, Benefits, and Career Growth Survey Questions
Sample questions
How satisfied are you with your overall compensation relative to your role and responsibilities?
How satisfied are you with the benefits offered by the organization?
Do you believe compensation decisions are fair and transparent?
How satisfied are you with opportunities for professional development and continuing education?
Do you see a clear path for career growth within this organization?
Fairness shapes retention just as much as the paycheck itself
Why & When to Use
Use this survey type when you want to understand whether providers feel appropriately rewarded, supported by benefits, and able to build a future inside your organization.
It is especially useful when hiring feels like pulling teeth, turnover is climbing, or providers are openly frustrated about pay equity, incentives, or advancement.
Here’s the thing: people do not judge compensation on salary alone.
They also look at fairness, transparency, benefits, growth opportunities, and whether the whole package matches the demands of the job.
This survey works well during compensation reviews, benefit redesigns, workforce planning, or professional development discussions.
On top of that, it helps you spot whether the real issue is base pay, bonus structure, benefits value, or a career ladder that looks more like a trapdoor.
A few practical ways to make this survey more useful:
Separate questions about pay, benefits, incentives, and career growth so you get clear, actionable feedback.
Pay attention to perceived fairness, because providers may react as strongly to opaque decisions as to low compensation.
Interpret results with specialty, market, or regional comparisons where relevant, especially in hard-to-recruit roles.
Avoid vague compensation questions unless you are prepared to explain findings, review policies, and respond with real next steps.
Provider Clinical Support and Administrative Processes Survey Questions
Sample questions
How satisfied are you with the usability of the EHR and other clinical systems?
Do administrative processes help or hinder your ability to provide patient care?
How satisfied are you with the responsiveness of support teams such as IT, billing, or scheduling?
How efficient are referral, prior authorization, and care coordination workflows?
Do you have the tools and resources needed to deliver high-quality care?
Operational friction can drain provider energy faster than a packed waiting room
Why & When to Use
Use this survey type when you want to see how systems, tools, and workflows affect providers’ ability to care for patients efficiently.
It is especially useful when providers keep grumbling about paperwork, EHR clicks, referral bottlenecks, or support teams that move at the speed of wet cement.
Here’s the thing: even highly committed providers can burn out when daily processes make simple tasks feel weirdly heroic.
That is why this survey works well during operational improvement projects, workflow redesign, documentation reduction efforts, or broader care-delivery changes.
A few ways to make this survey more useful:
Ask about specific pain points like charting, prior authorizations, referrals, inbox management, scheduling, and billing support, not just broad process satisfaction.
Pair survey results with operational metrics such as documentation time, authorization turnaround, referral completion rates, or support response times.
Look for repetitive tasks that steal provider time, because removing one annoying step can sometimes do more good than launching a shiny new initiative.
Prioritize fixes that reduce manual effort, improve handoffs, and make it easier for providers to focus on patient care instead of administrative gymnastics.
Best Practices for Writing and Using Provider Satisfaction Survey Questions
Sample questions
Are the survey questions specific enough to reveal actionable issues?
Does the survey use neutral wording that avoids biasing responses?
Can providers complete the survey quickly without fatigue?
Are open-ended questions included to capture context behind ratings?
Is there a clear plan for sharing findings and acting on results?
Good survey design turns opinions into useful decisions
Why & When to Use
Use this section as your go-to framework before launching any provider satisfaction survey.
It helps you build questions that get honest feedback, point to clear next steps, and give you results you can actually compare over time.
Here’s the thing: a messy survey creates messy data, and no one wants to make big decisions with guesswork wearing a lab coat.
This section is especially useful for HR leaders, medical directors, practice administrators, and healthcare operations teams that need feedback to be both credible and practical.
A few best practices matter most:
Keep surveys short, focused, and tied to a clear purpose.
Use plain, neutral wording so you measure real opinions, not your own assumptions.
Protect anonymity when possible, because people are usually more candid when they do not feel watched.
Segment results by meaningful groups like specialty, location, or employment type.
Keep core questions consistent over time so you can spot trends.
Share findings and explain what actions will follow.
And a few traps to avoid:
Do not ask double-barreled questions.
Do not bury meaning under jargon or vague wording.
Do not survey providers without leadership support and a response plan.
Do not ignore written comments, because that is often where the real story is hiding.
How to Analyze Provider Satisfaction Survey Results
Sample questions
Which survey items have the lowest satisfaction scores?
Which issues show the largest gaps between importance and satisfaction?
Are there major differences by specialty, site, tenure, or provider type?
What themes appear repeatedly in open-ended comments?
Which problem areas are most closely linked to retention risk or burnout?
Smart analysis turns feedback into priorities you can actually act on
Why & When to Use
Use this section when you already have survey results but need help turning a pile of responses into a clear action plan.
It is especially useful right after a survey cycle and before you decide what to fix first.
Here’s the thing: averages can be helpful, but they can also hide the real story like a toddler hiding behind a curtain with their feet sticking out.
Start by looking beyond overall scores.
Review trends over time, not just one survey snapshot.
Compare results against internal benchmarks or past cycles.
Break data out by specialty, site, tenure, and provider type.
Read open-ended comments for repeating themes and context.
Cross-reference findings with turnover, absenteeism, patient access, and quality indicators.
Plus, separate issues into two buckets so your next steps are easier to manage.
Quick wins are problems you can solve fast, like communication gaps or scheduling confusion.
Structural issues are bigger challenges, like staffing shortages, leadership trust, or workflow design.
On top of that, be careful with small sample sizes.
Do not overreact to tiny score changes or subgroup differences unless the pattern is consistent, meaningful, and backed up by comments or operational data.
Turning Provider Survey Insights Into Action
Sample questions
What are the top three issues providers want addressed first?
Which actions can leadership realistically take in the next 30, 60, and 90 days?
Who is accountable for each improvement initiative?
How will progress be communicated back to providers?
When will the organization re-survey to measure improvement?
Feedback only matters when you turn it into visible change
Why & When to Use
Use this wrap-up section when you want to help readers move from survey findings to real improvement efforts people can actually see.
It works best as the conclusion because it reinforces the big point: surveys are not the finish line, they are the starting whistle.
Here’s the thing: if providers take time to give honest feedback and nothing happens, trust drops fast.
Plus, when leaders follow through in clear, visible ways, future survey response rates usually improve because people can tell their input did not vanish into a PowerPoint abyss.
Turn insights into a simple action plan that names what will happen, who owns it, and how success will be measured.
Prioritize the top issues providers want addressed first.
Set realistic 30, 60, and 90 day actions.
Assign an owner to every initiative.
Define measurable outcomes so progress is easy to track.
Share updates regularly so providers know what is changing.
On top of that, use pulse surveys to check whether your fixes are actually working.
A short follow-up survey can tell you if communication improved, workflows got easier, or frustration is still hanging around like an uninvited guest.
End strong: provider satisfaction surveys should build trust, support retention, and improve care, not just generate reports that collect digital dust.
Related Employee Survey Surveys
29 Essential Post Mortem Survey Questions for Project Success
Discover 25+ essential post mortem survey questions to improve projects, boost team morale, and d...
28 Change Readiness Survey Questions to Assess Organizational Adaptability
Discover 25 sample change readiness survey questions to assess your team's preparedness for chang...
28 Retreat Survey Questions to Boost Your Event Feedback
Explore 25 retreat survey questions to boost feedback and plan better retreats. Discover top samp...