31 Health Insurance Survey Questions to Ask Customers
Explore 25 health insurance survey questions to assess coverage, satisfaction, and value. Read expert sample questions and insights.
Health insurance surveys give you a practical way to hear what people actually think about coverage, costs, enrollment, and claims. A smart health insurance questionnaire helps employers, insurers, and healthcare teams spot confusion before it turns into frustration. When you collect feedback from employees, policyholders, or patients using an online survey tool, you can improve plan design, manage costs, support compliance, and make better decisions about benefits benchmarking, open enrollment, provider networks, and more. In short, a well-built medical insurance survey turns guesswork into action.
Employee Health Insurance Satisfaction Survey
Why & When to Use
Employee sentiment tells you where benefits shine and where they quietly annoy people.
If you want to know how your health plan is landing with your team, this is the survey to use.
An employee health insurance satisfaction survey works best when you send it mid-year or soon after open enrollment, while experiences are still fresh and before the next renewal cycle sneaks up on you.
For HR teams, this type of health insurance evaluation survey is a reality check.
You may think a plan looks competitive on paper, but your employees might be wrestling with high deductibles, limited networks, or prescription costs that make them wince a little.
Here’s the thing, benefits are not just a budget item.
They shape how supported people feel at work, and they can influence retention more than many leaders expect.
A good health insurance survey for employees helps you learn whether your plan is easy to use, easy to understand, and worth the money from the employee perspective.
That insight gives you something far more useful than assumptions.
It gives you direction.
Use this survey when you need to:
Measure overall satisfaction with current health benefits.
Identify pain points before renewal discussions begin.
Compare employee feedback across departments, locations, or plan tiers.
Understand whether cost sharing is causing employees to delay care.
Learn how benefits affect loyalty and retention.
Plus, this survey can uncover emotional signals, not just operational ones.
If your people feel confused or financially stretched, that often shows up here first.
And yes, health benefits can inspire dramatic feelings, because nothing says “fun Tuesday” like trying to decode a deductible.
Sample Questions
When you write employee health insurance survey questions, keep the wording simple and direct.
Most questions work well on a 5-point Likert scale, with one NPS-style question and one single-choice item to add variety.
Use this exact set if you want a strong starting point for your health insurance survey questionnaire:
How satisfied are you with the overall value of your current employee health insurance plan?
Which plan feature (premium, deductible, network size, prescription coverage) do you feel needs the most improvement?
How easy was it to understand plan options during benefits enrollment?
In the past 12 months, have you delayed care due to out-of-pocket costs?
How likely are you to stay with our company because of its health benefits?
These questions work because they cover value, usability, affordability, and retention in one tidy package.
On top of that, they help you separate general unhappiness from specific fixable issues.
For example, if employees say they are unhappy with value, the second question tells you whether premiums, deductibles, network size, or drug coverage are doing the damage.
If many employees report delaying care, you have a red flag that cost-sharing may be hurting both wellbeing and long-term claims outcomes.
That is the kind of signal no employer should shrug off.
A medical insurance survey like this also gives you trends you can track over time.
If understanding improves after you simplify enrollment materials, great.
If loyalty scores stay flat even after a plan update, you know there is more work to do.
In the Commonwealth Fund’s 2023 survey, 54% of people with employer coverage who delayed or skipped care due to costs said their or a family member’s health worsened (source)
How to create a survey in HeySurvey
1. Create a new survey
Start by opening HeySurvey and choosing a way to begin: use an empty sheet, pick a pre-built template, or type your questions directly and let HeySurvey format them for you. If you’re already on this page, you can also click the button below to open a template and get started right away. Once the survey opens in the editor, give it a clear internal name so you can easily find it later.
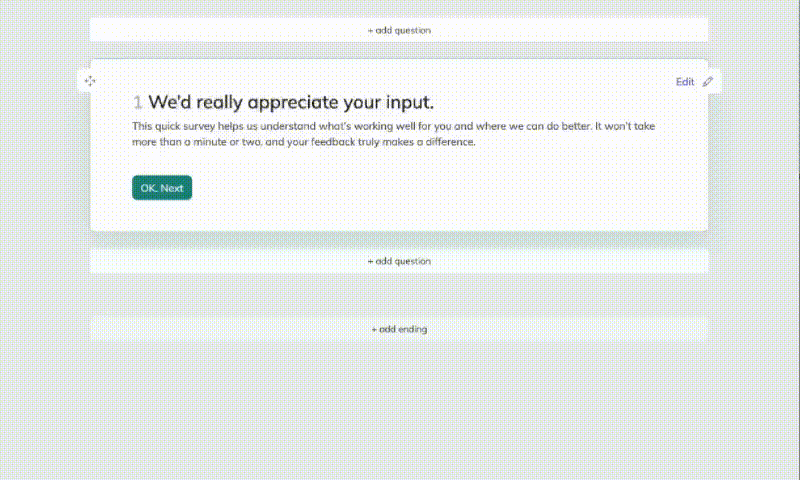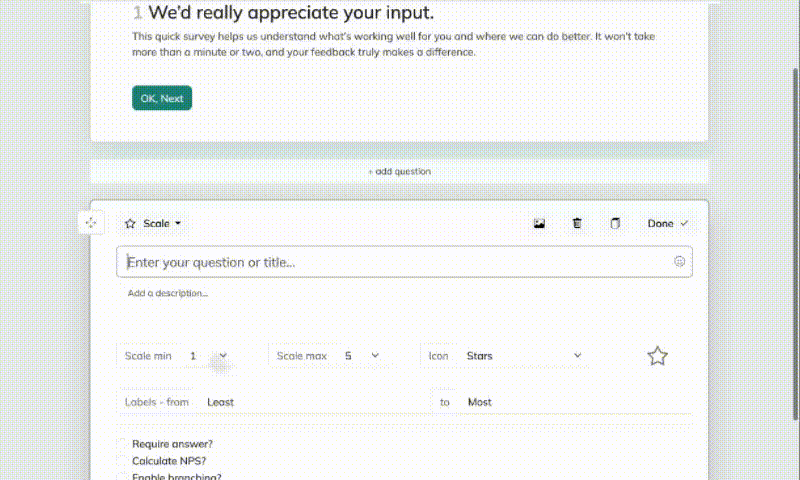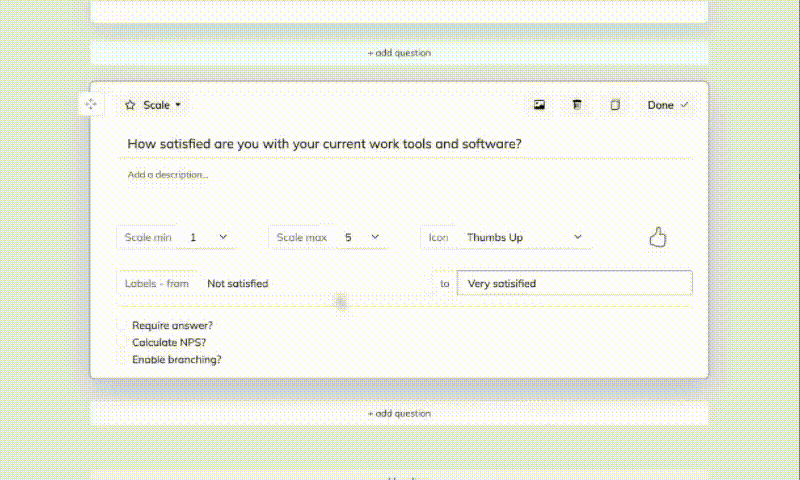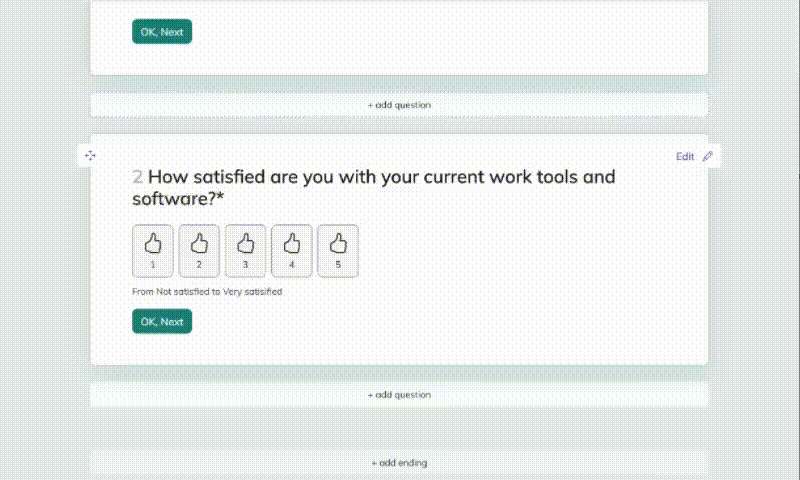
2. Add questions
Click Add Question to insert your first question, then choose a question type such as text, choice, scale, number, dropdown, date, file upload, or statement. Add your question text, description, and any answer options you need. You can mark questions as required, duplicate them to save time, and even add images to questions or answer choices. If your survey needs a guided flow, set up branches so respondents move to different questions based on their answers.
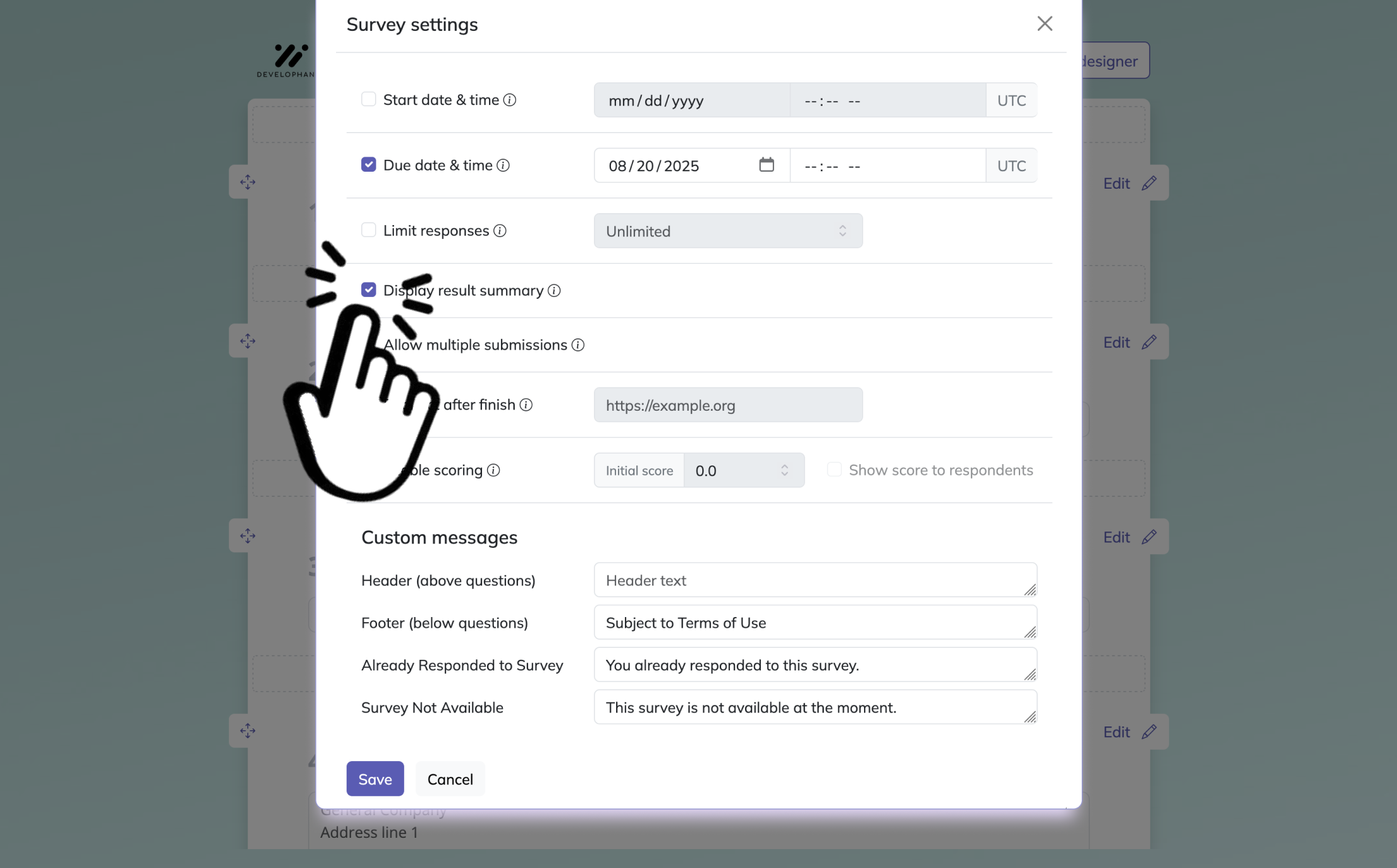
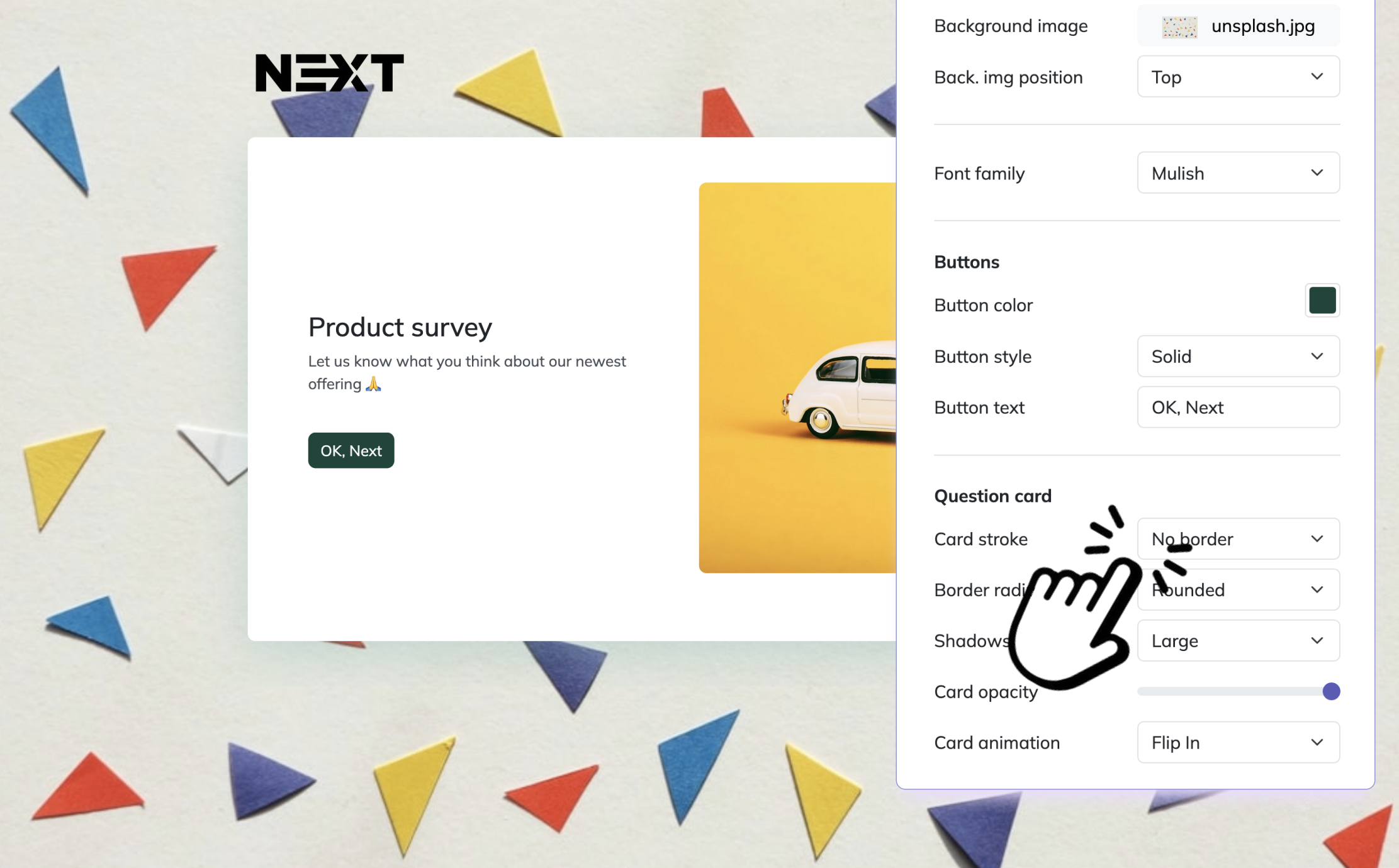
Bonus steps: apply branding and settings
Before publishing, you can make the survey look like your own by adding a logo and using the Designer Sidebar to adjust colors, fonts, backgrounds, layouts, and animations. In the Settings panel, you can set start and end dates, limit responses, add a redirect URL, or choose whether respondents can view results.
3. Publish your survey
Preview your survey first to see it exactly as respondents will. When everything looks right, click Publish to generate a shareable link. Publishing requires an account, so you can save responses and view results later.
Health Insurance Enrollment & Onboarding Survey
Why & When to Use
First impressions of coverage often happen during enrollment, not at the doctor’s office.
That is why the enrollment and onboarding phase deserves its own survey.
A health insurance questionnaire sent right after someone completes enrollment helps you spot friction points while the process is still fresh in their mind.
This is especially useful for employers, insurers, and benefits administrators that want to improve self-service and reduce support requests.
When people struggle with enrollment, they often do one of three things.
They call support, choose the wrong option, or give up halfway through and mutter at their screen.
None of those outcomes is ideal.
Use this health insurance survey after new hires enroll, after annual benefits selection wraps up, or after policyholders complete digital onboarding.
The goal is to understand whether the experience felt clear, fast, and confidence-building.
If users do not understand eligibility, deadlines, required forms, or what happens next, the cracks will show here.
This survey can help you improve:
Eligibility messaging and step-by-step instructions.
Portal design and mobile usability.
Delivery of policy documents and confirmation materials.
New member confidence in using their coverage.
Call-center volume caused by preventable confusion.
Here’s the thing, the best onboarding does not just move people through a form.
It makes them feel informed and ready to use their benefits.
That matters because confusion during enrollment tends to linger.
If someone starts off uncertain, they are more likely to remain uncertain when they need care.
A well-timed health insurance evaluation survey lets you fix that early.
Sample Questions
For this survey, your questions should focus on clarity, speed, and readiness.
You want to know where people hesitated, what felt clunky, and whether they ended the process feeling confident instead of mildly bewildered.
Use these sample questions in your medical insurance survey:
How clear were the eligibility requirements presented during enrollment?
Rate the simplicity of the online enrollment portal.
Which step in the enrollment journey felt most time-consuming?
Did you receive all required policy documents within five business days?
How confident do you feel about using your coverage after onboarding?
This set gives you both measurable feedback and useful texture.
Closed-ended questions help you benchmark performance, while the open-ended question points directly to the slowest or most frustrating step.
Plus, confidence after onboarding is a powerful metric.
If people finish enrollment but still feel unsure how to use their plan, your process may be technically complete but not truly successful.
That distinction matters.
A strong health insurance survey questionnaire should reveal whether your digital journey is intuitive or just survivable.
If respondents consistently mention document uploads, account setup, or plan comparison as painful steps, those become your priority fixes.
Small tweaks can make a big difference here.
Clearer labels, shorter forms, better progress indicators, and faster document delivery can reduce friction fast.
And when people do not need to call support just to understand what they selected, everyone wins.
KFF found 29% of insured adults had difficulty understanding their health insurance explanation of benefits, underscoring the need for clear enrollment and onboarding survey questions. Source
Medical Claims Experience Survey
Why & When to Use
Claims are where trust gets tested in real time.
You can promise good service all day, but the claims experience is where members decide whether they believe you.
That is why a medical claims experience survey should be sent about 7 to 10 days after a claim is processed.
At that point, the interaction is recent enough for details to be remembered, but settled enough for people to reflect on the full experience.
A claims-focused health insurance survey helps you understand more than reimbursement speed.
It also shows whether members found the process fair, clear, and easy to navigate.
If your Explanation of Benefits is confusing, if reimbursements feel inconsistent, or if support interactions are frequent and frustrating, this survey will bring those issues into daylight.
Use it to monitor:
Satisfaction with reimbursement speed.
Clarity of claims communication and EOB language.
Frequency of support contact after a claim.
Perceived fairness of claim outcomes.
Willingness to recommend the claims experience.
Here’s the thing, claims are emotional.
People are often dealing with illness, treatment, bills, and stress at the same time.
So even a small delay or a vague message can feel much bigger than it might in another customer journey.
A strong health insurance evaluation survey in this area helps you reduce friction where it matters most.
And if your claims process is smooth, clear, and fair, members are much more likely to stick around.
No one throws confetti over an EOB, but a painless claims experience comes surprisingly close.
Sample Questions
Your claims questions should be direct and easy to answer.
This is not the time for vague wording or industry jargon that sounds like it was written by a committee in a windowless room.
Use these questions about health insurance claims:
How satisfied are you with the speed of your most recent claim reimbursement?
Was the Explanation of Benefits (EOB) easy to understand?
Did you need to contact support to resolve any claim issues?
Rate the fairness of the amount you were reimbursed.
How likely are you to recommend our claims service to others?
These questions work well because they move from process to perception.
First, you learn whether the claim moved quickly.
Then, you find out whether communication was clear, whether extra effort was required, whether the payment felt fair, and whether the overall experience was strong enough to recommend.
On top of that, this structure helps you identify exactly where trust breaks down.
A low recommendation score paired with good speed but poor EOB clarity points to a communication problem.
A high support-contact rate suggests your process may be creating unnecessary confusion or forcing members to chase answers.
This kind of health insurance survey data is especially useful when comparing claim types, service lines, or regional performance.
If one category consistently scores lower, you can investigate whether denials, documentation requirements, or vendor workflows are driving the difference.
That is much more useful than just hearing people are unhappy and hoping it sorts itself out.
Provider Network Accessibility Survey
Why & When to Use
A plan can look excellent on paper and still fail if care is hard to reach.
That is why provider network accessibility deserves focused attention.
A provider network accessibility survey helps you understand whether members can actually find and use in-network care where they live.
This type of medical insurance survey is especially useful when you are adding or removing physicians, expanding into new regions, or reviewing access gaps on a quarterly basis.
You want to know if members can find primary care nearby, schedule specialists without epic delays, and avoid surprise bills caused by network confusion.
If the answer is no, costs rise and satisfaction sinks.
That is not just frustrating for members.
It can also create avoidable out-of-network spending and damage trust in the plan.
Use this health insurance questionnaire to assess:
Access to in-network primary care within a reasonable distance.
Availability of specialists by region.
Frequency of surprise billing tied to network issues.
Satisfaction with telehealth options.
Wait times for in-network appointments.
Plus, provider access is one of those topics that people notice fast.
They might not remember every plan detail, but they definitely remember driving too far, waiting too long, or getting a bill they did not expect.
That kind of experience sticks.
A good health insurance survey questionnaire helps you pinpoint whether the issue is geography, directory accuracy, specialty shortages, or poor communication about network status.
And yes, nothing says “customer delight” quite like discovering your carefully chosen doctor was somehow out of network after all.
Sample Questions
Your survey questions should focus on actual access, not just general satisfaction.
You want practical answers that show whether members can find the right care at the right time without turning it into a scavenger hunt.
Use these sample questions:
How easy is it to find in-network primary care providers within 15 miles of your home?
Have you experienced surprise bills due to out-of-network services?
Rate the availability of specialists (e.g., dermatology, cardiology) in your area.
How satisfied are you with telehealth options offered under your plan?
What is the longest wait time you’ve encountered when scheduling an in-network appointment?
This question set balances ease, availability, billing surprises, and convenience.
It also helps you see whether telehealth is filling network gaps or simply sitting there looking helpful in theory.
Here’s the thing, geography alone does not tell the whole story.
A provider may be technically in network but unavailable for weeks, not accepting new patients, or listed incorrectly.
That is why the wait-time question matters so much.
It gives you a real-world view of access rather than a glossy one.
When enough respondents report long specialist waits or surprise bills, that is your cue to review contracts, directory accuracy, and regional coverage strategy.
A health insurance evaluation survey in this area can help reduce cost leakage and improve care access at the same time.
A 2024 study found callers secured appointments with just 3.9% of listed ACA mental health providers, highlighting why accessibility surveys should measure real network access, not directory listings alone (source)
Plan Coverage & Benefits Comprehension Survey
Why & When to Use
If people do not understand their benefits, they cannot use them well.
Coverage comprehension is one of the most overlooked parts of a strong health insurance experience.
A plan may include valuable preventive services, mental health support, prescription benefits, or wellness perks, but if members do not understand how those features work, much of that value goes unused.
That is where a plan coverage and benefits comprehension survey comes in.
This type of health insurance questionnaire is best sent before open enrollment or right after major policy updates.
It helps you learn whether people understand common terms like deductible, co-insurance, and out-of-pocket maximum, and whether your education materials are doing their job.
If they are not, members may make poor plan choices or avoid care because they assume it will cost more than it actually does.
Use this health insurance survey to evaluate:
Confidence in explaining basic plan terms.
Areas of benefits confusion.
Awareness and use of the summary of benefits and coverage.
Helpfulness of educational materials.
Requests for additional information or guidance.
On top of that, this survey supports smarter communication.
If many members struggle with the same concepts, you know exactly where to simplify language, add examples, or improve enrollment support.
Health insurance already has enough acronyms to make anyone’s eyes glaze over.
You do not need your education materials adding to the drama.
Sample Questions
The best questions in this section are simple, specific, and tied to real understanding.
You are not testing people for fun.
You are checking whether your communication made complicated ideas feel manageable.
Use these sample questions:
How confident are you in explaining your deductible to a colleague?
Which benefit area (preventive care, mental health, maternity, prescriptions) is least clear to you?
Have you accessed the summary of benefits and coverage (SBC) in the past six months?
Rate the usefulness of our benefits education materials.
What additional information would help you better understand your coverage?
These questions reveal both confidence and knowledge gaps.
If respondents say they are not confident explaining a deductible, that is a strong sign your materials may be too abstract or too dense.
If a specific benefit area keeps showing up as unclear, that tells you where to focus your next communication push.
Plus, the open-ended question is especially valuable here.
People will often tell you exactly what would help, whether that is plain-language examples, short videos, side-by-side comparisons, or clearer cost scenarios.
That kind of feedback is gold.
A health insurance survey questionnaire in this category helps you move from dumping information on people to actually helping them understand it.
And when understanding improves, decision-making usually improves right along with it.
Cost & Value Perception Survey
Why & When to Use
People do not judge a plan by price alone, but price definitely gets invited to the conversation.
A cost and value perception survey helps you understand whether members feel the plan is worth what they pay.
This kind of health insurance evaluation survey is best conducted annually, especially ahead of premium changes, renewal planning, or benefit redesign discussions.
You are trying to measure more than affordability.
You are also measuring perceived fairness, trade-offs, and whether wellness incentives or covered services meaningfully offset costs.
Two people can pay the same premium and feel very differently about value.
One may see strong protection and useful benefits.
The other may see a monthly charge paired with too many bills after care.
That gap matters.
Use this medical insurance survey to explore:
Satisfaction with premium-to-coverage ratio.
Sensitivity to premium increases.
Which cost element causes the most concern.
Whether incentives reduce financial strain.
Overall sense of value for money.
Here’s the thing, value is emotional as much as mathematical.
Members compare what they pay with what they can access, what they understand, and how much financial stress the plan creates when care is needed.
If costs feel unpredictable, value usually drops, even if the plan is technically competitive.
This is why a health insurance survey should never look only at premiums.
Deductibles, co-pays, and out-of-pocket maximums all shape perception.
And if your members need a spreadsheet, a calculator, and a calming cup of tea just to estimate expenses, that is useful feedback in itself.
Sample Questions
The questions in this section should help you identify pressure points and trade-off tolerance.
You want to know what cost changes members might accept, what they fear most, and whether the current structure feels reasonable.
Use these sample questions:
How satisfied are you with the ratio of monthly premium to coverage received?
If premiums increased by 5%, how likely would you be to switch plans?
Which cost element concerns you the most? (premium, deductible, co-pay, out-of-pocket max)
Do wellness incentives offset any of your healthcare expenses?
Overall, do you feel your plan delivers good value for the money you pay?
This set gives you a strong mix of present perception and future risk.
The first and fifth questions measure overall value from slightly different angles, while the second question estimates churn sensitivity if costs rise.
The third question helps you pinpoint the exact financial pain point.
That matters because not all cost complaints mean the same thing.
Some members can handle a higher premium if care is more predictable.
Others prefer lower monthly costs and are willing to take on more risk later.
Your survey results can help you understand these preferences instead of guessing.
Plus, if wellness incentives are barely moving the needle, you may need to redesign them or explain them better.
A smart health insurance survey questionnaire in this category helps you align pricing strategy with what members actually experience, not just what plan documents say.
Health Insurance Renewal & Retention Intent Survey
Why & When to Use
Renewal intent tells you what people are planning before they quietly leave.
A renewal and retention intent survey is one of the clearest ways to forecast future behavior.
Send it 60 to 90 days before renewal, and you can gauge how likely members are to stay, what would influence that decision, and whether they are already browsing alternatives.
This is useful for employers preparing for benefit changes and for insurers trying to reduce churn.
A health insurance survey at this stage helps you move from reactive to proactive.
Instead of waiting for non-renewals to pile up, you can identify at-risk groups early and respond with better communication, plan adjustments, or targeted offers.
That timing is the whole game.
Once someone has mentally checked out, winning them back gets much harder.
Use this health insurance questionnaire to understand:
Likelihood of renewal.
Key improvements that would influence retention.
Whether members are comparing other options.
Clarity of communication about plan changes.
Preference for premium versus out-of-pocket trade-offs.
Plus, this survey is especially powerful when paired with earlier feedback from satisfaction, claims, and cost surveys.
It helps connect past experience with future action.
If low value scores, poor access, and weak communication all show up alongside low renewal intent, the story becomes very clear.
People are not just mildly annoyed.
They are preparing to leave.
And yes, they may be comparison-shopping with the efficiency of someone hunting for the last good parking spot.
Sample Questions
Renewal questions should be practical, focused, and easy to compare over time.
You want enough detail to act on, but not so much that the survey becomes one more thing people avoid until “later,” which of course means never.
Use these sample questions:
How likely are you to renew your current health insurance plan?
What single improvement would most influence your decision to stay?
Are you actively comparing alternative medical insurance options?
Rate the clarity of communication regarding upcoming plan changes.
Do you prefer a higher premium with lower out-of-pocket costs or vice versa?
These questions give you both forecast and context.
The likelihood-to-renew score shows your overall retention picture, while the open-ended improvement question tells you what matters most to members right now.
The comparison-shopping question is especially useful because it signals active risk.
If many respondents are already exploring alternatives, you may need to step up communication or revisit plan positioning fast.
On top of that, the preference question helps you understand what kind of plan design people may favor at renewal.
A health insurance evaluation survey in this phase can shape messaging, pricing strategy, and benefit design in a very direct way.
That makes it one of the most actionable surveys in the whole cycle.
Best Practices & Dos and Don’ts for Crafting High-Impact Health Insurance Surveys
Dos
Good survey design makes honest feedback easier to give and easier to use.
If you want reliable responses, your survey has to feel simple, relevant, and respectful of people’s time.
The best health insurance surveys are built with clear language, smart timing, strong privacy habits, and a plan for what happens after the data comes in.
Start with wording that real people can understand.
Health insurance terms can get dense fast, so keep your questions jargon-free unless the audience already knows the language well.
Mix closed and open-ended formats so you can capture both measurable trends and useful explanations.
Time your surveys strategically.
A claims survey works after a claim, an onboarding survey works after enrollment, and a renewal survey works before renewal.
Send the right survey at the right moment, and the feedback becomes much more accurate.
Make sure your process protects privacy and respects HIPAA and PHI requirements where applicable.
People are far more likely to answer honestly when they trust that sensitive information is being handled properly.
Benchmark results over time so you can see whether changes actually improve the experience.
Use these practices consistently:
Keep questions short, plain, and specific.
Match survey timing to the member or employee journey.
Optimize for mobile so people can respond without pinching and zooming like it is 2012.
Combine rating questions with a few open-text prompts.
Store feedback securely and limit access appropriately.
Review results by segment to find patterns across plans, groups, or regions.
Don’ts
A weak survey can create bad data even when response rates look fine.
That is why avoiding common mistakes matters just as much as following best practices.
Do not overload respondents with too many questions.
If a survey feels endless, people start speeding through it, abandoning it, or giving the same answer down the page just to escape.
Do not use biased wording.
Questions that push respondents toward a positive answer might look flattering at first, but they make the feedback less useful.
Ignore mobile optimization at your peril.
A health insurance survey questionnaire that is annoying on a phone will lose responses quickly.
Do not store survey data insecurely or mix sensitive feedback into systems without proper controls.
Trust is hard to win and easy to lose.
And finally, do not collect feedback and then do nothing with it.
People notice when surveys disappear into a black hole.
Avoid these missteps:
Asking too many questions in one sitting.
Writing leading or emotionally loaded items.
Using dense blocks of text instead of clean formatting.
Forgetting to test the survey on mobile devices.
Handling data without clear security safeguards.
Skipping follow-up actions or failing to communicate improvements.
Here’s the thing, the survey itself is only half the job.
The other half is showing people that their answers led to something better.
If you do that well, future response rates tend to rise, and the quality of insight improves too.
And that is a lovely little cycle to be in.
The strongest health insurance survey is the one that leads to action, not the one that just produces a very impressive spreadsheet.
Conclusion
Crafting effective health insurance survey questions transforms bland data into dynamic action. When organizations listen with intention, service levels climb, gaps shrink, and trust grows. Surveys connect voices with improvement and guide smart decisions all year long. No matter when you ask, the answers you uncover will always point the way forward. In the world of insurance, a single good question can change everything!
Related Customer Survey Surveys
29 Restaurant Survey Questions
Explore 25 restaurant survey questions with sample questions to improve feedback, service, and cu...

28 Airbnb Survey Questions to Improve Guest Experience
Discover 25 effective Airbnb survey questions to boost guest feedback and satisfaction. Enhance y...
29 Interior Design Survey Questions to Elevate Your Projects
Explore 25 top interior design survey questions to enhance your projects. Discover expert-crafted...